Insulin Resistance and Diabetes
Insulin resistance, a metabolic disorder characterized by impaired cellular response to insulin, underpins various chronic diseases, including type 2 diabetes and cardiovascular conditions. This scientific article explores the intricate molecular mechanisms of insulin resistance, elucidates its far-reaching implications for health, and delves into evidence-based therapeutic strategies that hold promise for its management.
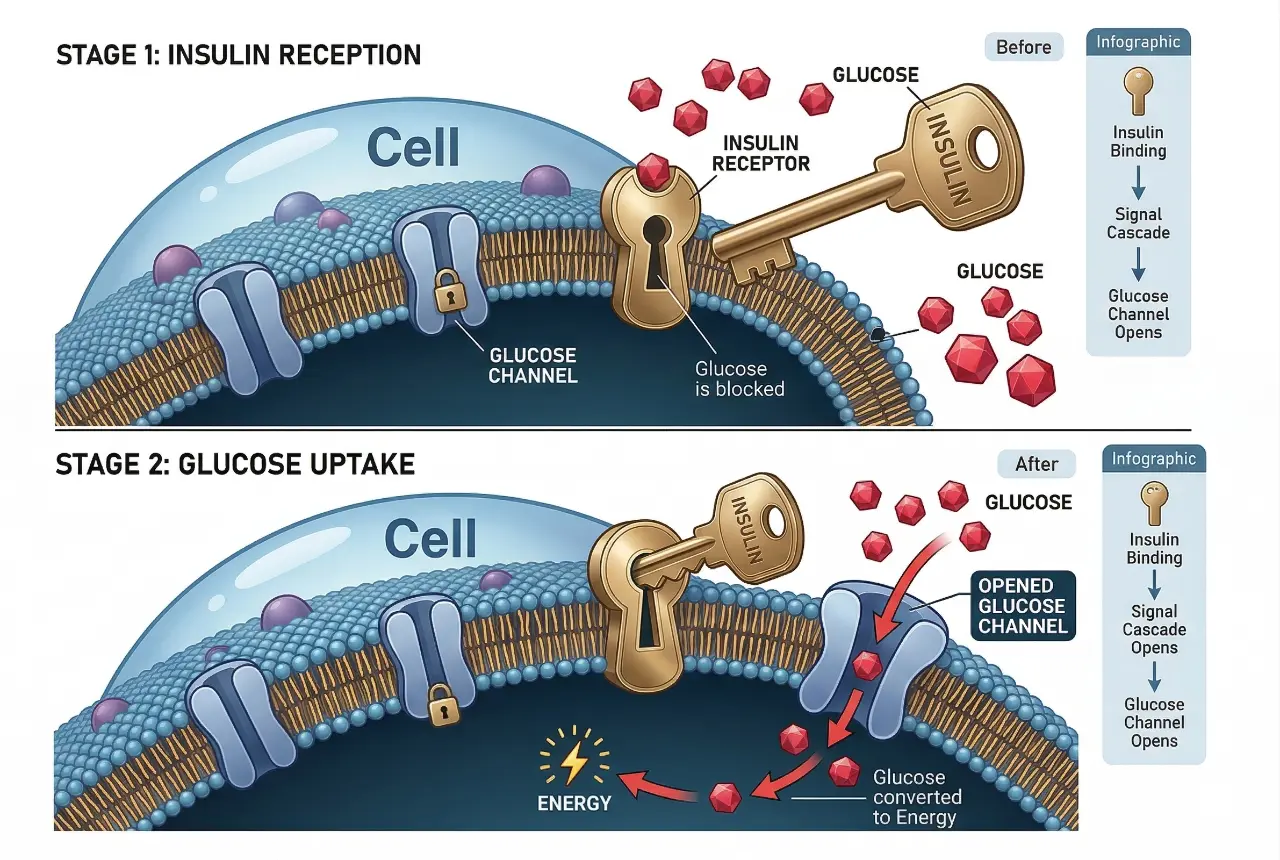
Insulin resistance is a central concern in contemporary healthcare, owing to its pervasive role in the development of type 2 diabetes mellitus (T2DM), obesity-related complications, and cardiovascular diseases. This article aims to unravel the multifaceted nature of insulin resistance by examining its molecular underpinnings, clinical significance, and therapeutic interventions grounded in scientific evidence.
Mechanisms of Insulin Resistance
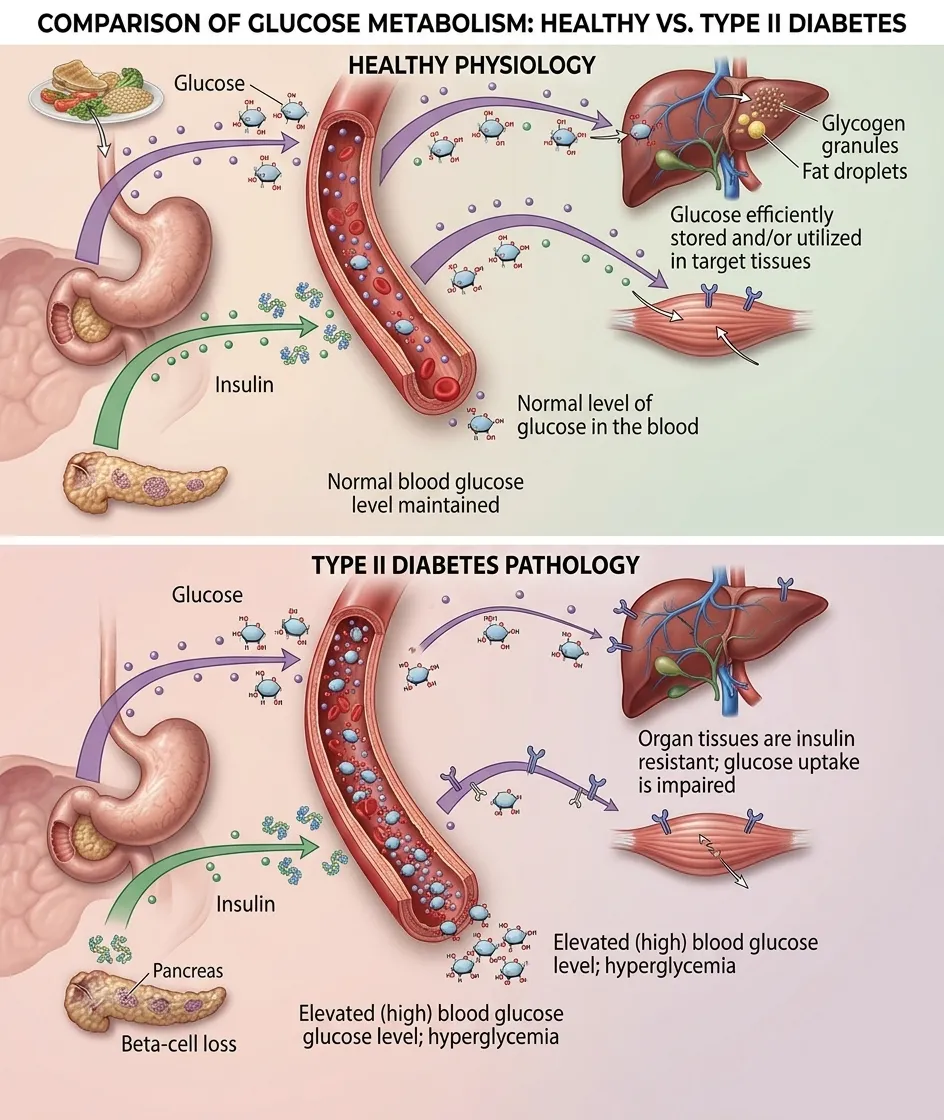
1. Adipose Tissue Dysfunction
Adipose tissue dysfunction contributes to insulin resistance through the dysregulated secretion of adipokines and the excessive release of free fatty acids (FFAs). Elevated FFAs induce lipotoxicity in non-adipose tissues, such as skeletal muscle and liver, thereby impairing insulin action[1][2].
2. Inflammatory Signaling
Chronic inflammation plays a pivotal role in the pathogenesis of insulin resistance. Cytokines like tumor necrosis factor-alpha (TNF-α) and interleukin-6 (IL-6) activate inflammatory pathways that interfere with insulin signaling cascades[3][4].
3. Mitochondrial Dysfunction
Mitochondrial abnormalities, including reduced oxidative phosphorylation capacity and increased oxidative stress, are associated with insulin resistance[5]. Impaired mitochondrial function contributes to reduced cellular energy metabolism, a key aspect of insulin-resistant states[6].
4. Endoplasmic Reticulum Stress
Endoplasmic reticulum (ER) stress arises from the accumulation of misfolded proteins within the ER. This phenomenon is observed in insulin-resistant cells and is linked to the disruption of insulin signaling[7][8].
Implications of Insulin Resistance

1. Type 2 Diabetes
Insulin resistance is a crucial precursor to T2DM. Skeletal muscle and liver insulin resistance leads to compensatory hyperinsulinemia. When the pancreatic beta cells can no longer maintain this compensatory response, impaired glucose homeostasis progresses to overt T2DM[9].
2. Cardiovascular Risk
Insulin resistance is a potent risk factor for cardiovascular diseases (CVDs). Dyslipidemia, hypertension, and endothelial dysfunction often accompany insulin resistance, promoting atherosclerosis and increasing the likelihood of myocardial infarctions and strokes[10][11].
3. Obesity
A bidirectional relationship exists between insulin resistance and obesity, where each condition exacerbates the other. Adipose tissue expansion and inflammation in obesity contribute significantly to insulin resistance[12].
4. Non-Alcoholic Fatty Liver Disease (NAFLD)
Insulin resistance in the liver is a primary driver of NAFLD. The reduced ability of insulin to suppress hepatic gluconeogenesis and promote lipid storage results in the accumulation of liver fat[13].
Therapeutic Strategies
1. Lifestyle Modifications
Lifestyle interventions encompassing dietary changes, regular physical activity, and weight management play a pivotal role in improving insulin sensitivity. Multiple studies have shown that exercise and dietary modifications can enhance insulin action and reduce insulin resistance[14][15].
2. Pharmacotherapy
Medications such as metformin, thiazolidinediones (TZDs), and glucagon-like peptide-1 (GLP-1) receptor agonists have demonstrated effectiveness in enhancing insulin sensitivity and improving glycemic control[16][17].
3. Personalized Medicine
Personalized approaches to insulin resistance management are emerging, with genetic and metabolic profiling offering insights into individualized treatment strategies[18].
4. Emerging Therapies
Ongoing research explores innovative therapies like sodium-glucose cotransporter-2 (SGLT-2) inhibitors and gut microbiota modulation for insulin resistance management[19][20].
5. Pulsed Electromagnetic Field (PEMF) as complementary therapy
Pulsed Electromagnetic Field (PEMF) therapy is an emerging modality that has shown promise in various medical applications, including the potential to improve insulin resistance. While more research is needed to fully understand the mechanisms and efficacy of PEMF for insulin resistance, several studies and theories suggest that PEMF may have beneficial effects in this context:
- Enhanced Cellular Function:
- Scientific Evidence: PEMF exposure may enhance cellular function by improving mitochondrial activity and increasing adenosine triphosphate (ATP) production[21]. Healthy mitochondrial function is critical for insulin sensitivity[22].
- Rationale: Enhanced mitochondrial activity can improve cellular energy metabolism, which plays a significant role in insulin sensitivity. This effect may potentially lead to improved glucose uptake and utilization in insulin-resistant cells.
- Anti-Inflammatory Effects:
- Scientific Evidence: PEMF therapy has been shown to reduce inflammation by modulating pro-inflammatory cytokines and promoting anti-inflammatory responses[23][24].
- Rationale: Chronic low-grade inflammation is a key contributor to insulin resistance[25]. By reducing inflammation, PEMF may help mitigate one of the underlying factors associated with insulin resistance.
- Improved Blood Flow:
- Scientific Evidence: PEMF therapy can enhance blood flow and microcirculation[26]. Improved circulation may promote nutrient and oxygen delivery to tissues, potentially benefiting insulin sensitivity.
- Rationale: Insufficient blood flow in adipose tissue and skeletal muscle has been linked to insulin resistance[27]. PEMF-induced improvements in circulation could help address this issue.
- Stress Reduction:
- Scientific Evidence: PEMF therapy has been associated with reduced stress and anxiety levels[28]. Stress is known to exacerbate insulin resistance[29].
- Rationale: By reducing stress, PEMF therapy may indirectly contribute to improved insulin sensitivity. Lower stress levels can lead to a decrease in cortisol secretion, a hormone that can promote insulin resistance when chronically elevated[30].
- Neurological Effects:
- Scientific Evidence: PEMF therapy may have positive effects on neurological function and neuroprotection[31].
- Rationale: Insulin resistance can impact the central nervous system and contribute to cognitive impairment[32]. If PEMF can support neurological function, it may indirectly improve insulin sensitivity.
It’s important to note that while these theoretical mechanisms suggest the potential benefits of PEMF therapy for insulin resistance, further clinical research is needed to confirm its effectiveness. Additionally, the optimal parameters, such as frequency, intensity, and duration of PEMF treatment for insulin resistance, need to be established through rigorous scientific investigation.
Nevertheless, PEMF therapy holds promise as a non-invasive and potentially beneficial approach for improving insulin resistance. Its ability to enhance cellular function, reduce inflammation, improve blood flow, and reduce stress may collectively contribute to better insulin sensitivity.
Conclusion
Insulin resistance is a multifaceted metabolic phenomenon with profound implications for health and well-being. Understanding its intricate molecular mechanisms and recognizing its clinical significance are essential steps in developing effective therapeutic strategies. Evidence-based interventions, including lifestyle modifications and pharmacotherapy, offer hope for ameliorating insulin resistance and reducing the risk of associated chronic diseases. The ongoing research landscape continues to uncover innovative approaches that hold the promise of a healthier future for individuals affected by insulin resistance.




















